Critical Information for Oral Health
GUM DISEASE
1. What is Gum Disease?
Gum Disease is a group of diseases that affect the gum and the bone surrounding our teeth.
There are two types of gum disease. The first is GINGIVITIS, which only affects the gums.
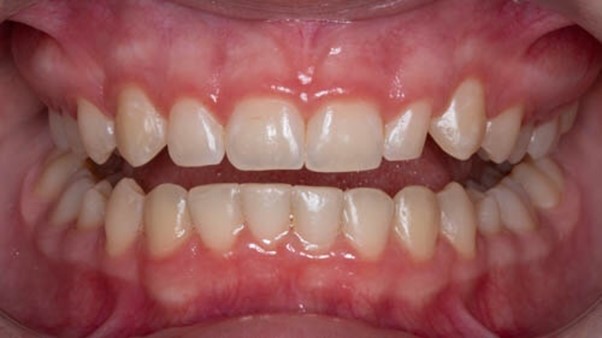
Gingivitis presents as swollen and bleeding gums when brushed or flossed. There is no damage to the bone supporting the tooth. If you improve the plaque removal, the gums return to health with no permanent damage. Gingivitis is the most common disease in the human body and affects most of the world’s population.
PERIODONTITIS
Periodontitis is a disease which could follow if gingivitis is not treated. It is essential to know that not ALL patients with gingivitis will progress to periodontitis.
The disease process involves the destruction of the bone and soft tissue that holds the tooth in place—creating a “pocket” between the gum and the tooth. The signs of periodontitis include bleeding gums (either with brushing, flossing or spontaneously), mobile teeth due to loss of bone, gum recession, temperature sensitivity, bad breath, drifting of teeth (resulting in gaps between those teeth), loss of gum between the teeth resulting in unsightly dark triangles. It is essential to realise that periodontal disease is painless and only becomes symptomatic when it is too late.
2. What causes Gum disease?
Gum disease is caused by bacteria that usually reside in the teeth. These bacteria live within dental plaque, a sticky substance containing mucous, food debris and millions of bacteria. The toxins produced by the bacteria are responsible for the infection that leads to signs and symptoms of gum disease. The bacteria that cause GINGIVITIS are different to the ones which cause PERIODONTITIS. If these bacteria are not removed by brushing and flossing daily, they stagnate and mature, becoming more aggressive and destructive over time. It takes about three months to develop into bacteria that can invade the gum space. The bacterial invasion sets the body’s immune response, which leads to the destruction of the bone, soft tissue and ligament supporting the tooth.
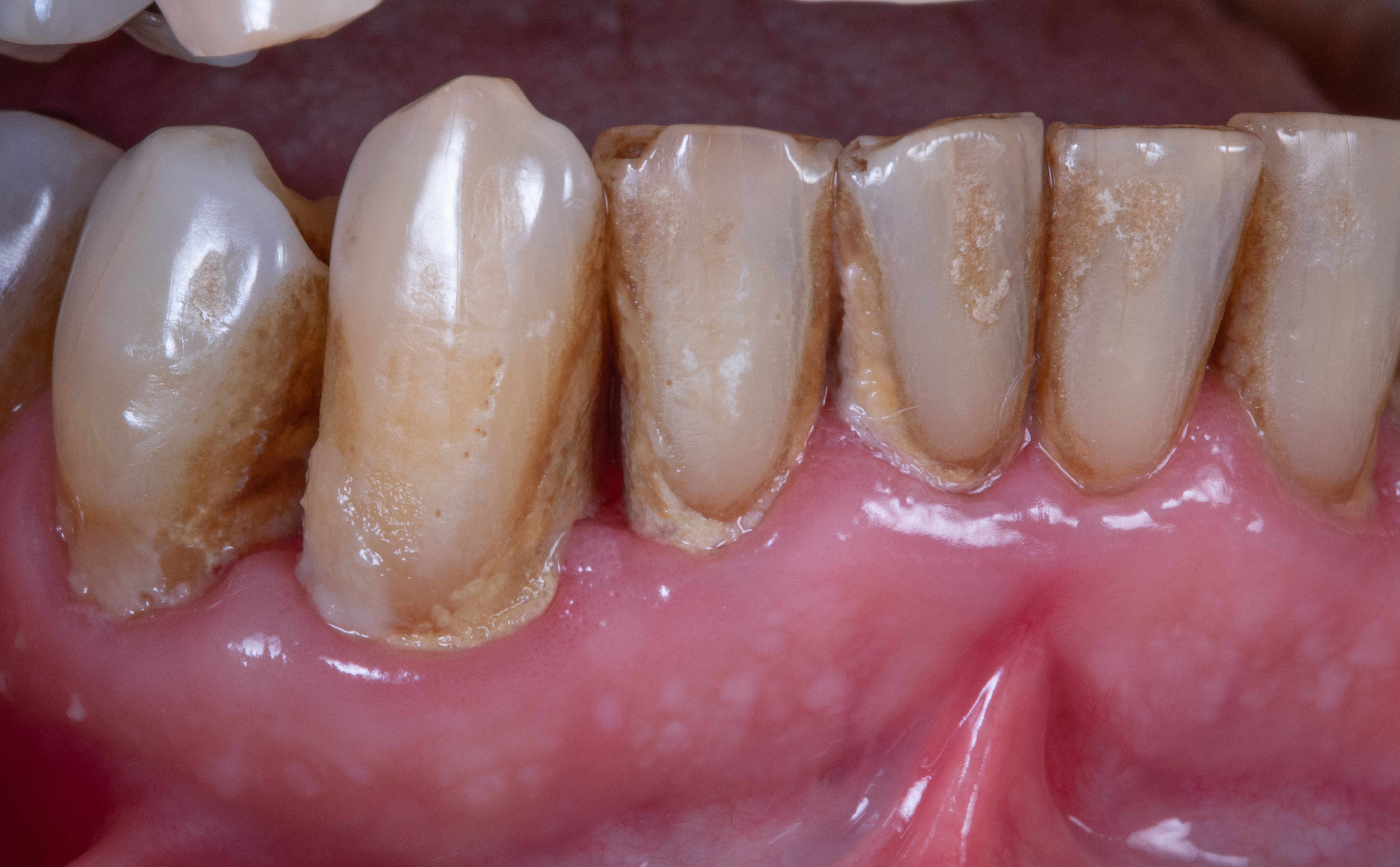
3. Are there any diseases, conditions or habits that may predispose me to; or aggravate gum disease?
Multiple situations will predispose people to get gum disease. And other scenarios which will determine the severity of the disease. Firstly, there is genetic susceptibility. This means that if you have the wrong genes (inherited from a family member), you are more likely to get periodontitis and the severity of the disease is generally worse. Secondly, the type of bacteria that grow will determine whether you get bone destruction and the severity of the destruction. Thirdly, certain diseases make periodontitis worse, and the most severe offender is diabetes. Periodontitis is a recognised complication of long-term diabetic illness. Untreated periodontitis can also impact the ability of a person with diabetes to control their blood sugar. If you have diabetes, making sure you visit your dentist, periodontist and hygienist are critical for your long-term health. Smoking is the last factor affecting disease severity and the ability to control it. The heavier you smoke, the more at risk you are and the more difficult it becomes to treat the disease successfully.
4. Can gum disease affect my overall health?
Periodontitis has been strongly linked to several systemic diseases, for example, heart disease, low birth weight and preterm babies, pneumonia, Alzheimer’s disease, diabetes and stroke. This means that if you have periodontitis, you are at a higher risk for one of these diseases.
5. How is gum disease treated?
The first step to treatment is diagnosing the disease. This is done by measuring the pockets created by gum disease with a special probe. X-rays further identify the bone loss around the teeth and are critical to the diagnostic process. Three-dimensional X-rays improve our ability to see the complete picture of bone loss. Bacterial DNA probes and genetic susceptibility testing allow us to determine further the risk of future bone loss and the predictability of treatment.
Treatment aims to remove the bacterial plaque, thereby reducing the inflammation in the gums. This is done by non-invasive deep cleaning and laser therapy in cases. The healing process will allow the gums to reattach to the tooth, thereby reducing the pocket. Unfortunately, the bone does not grow back. The treatment is best carried out by a person trained in the management of gum disease, like a periodontist or general dentist with special training. Oral hygienists are a significant factor in eliminating the disease and are crucial to preventing further disease breakdown. Meticulous oral hygiene is essential and will help keep the disease at bay.
Before and After Treatment
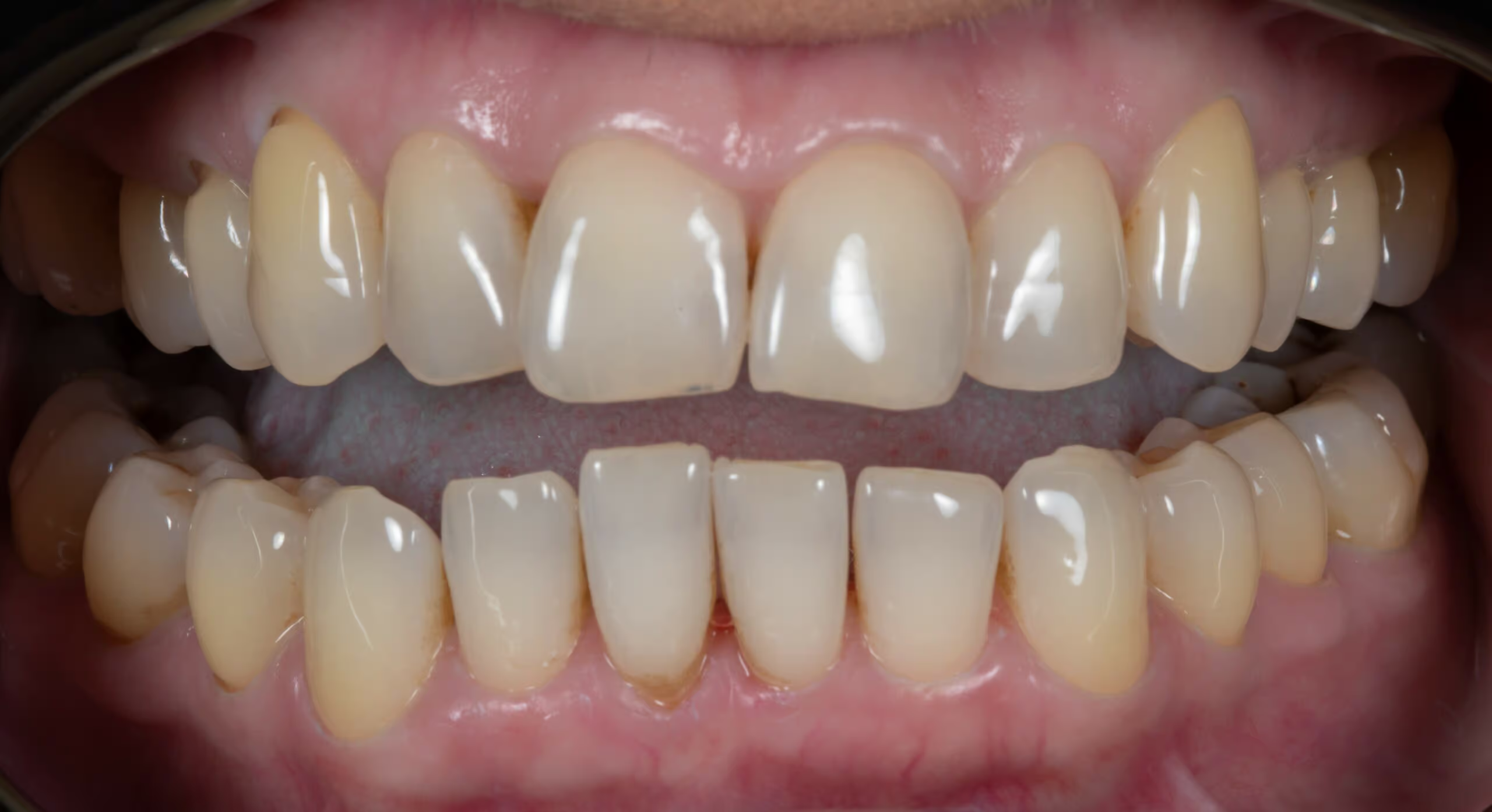
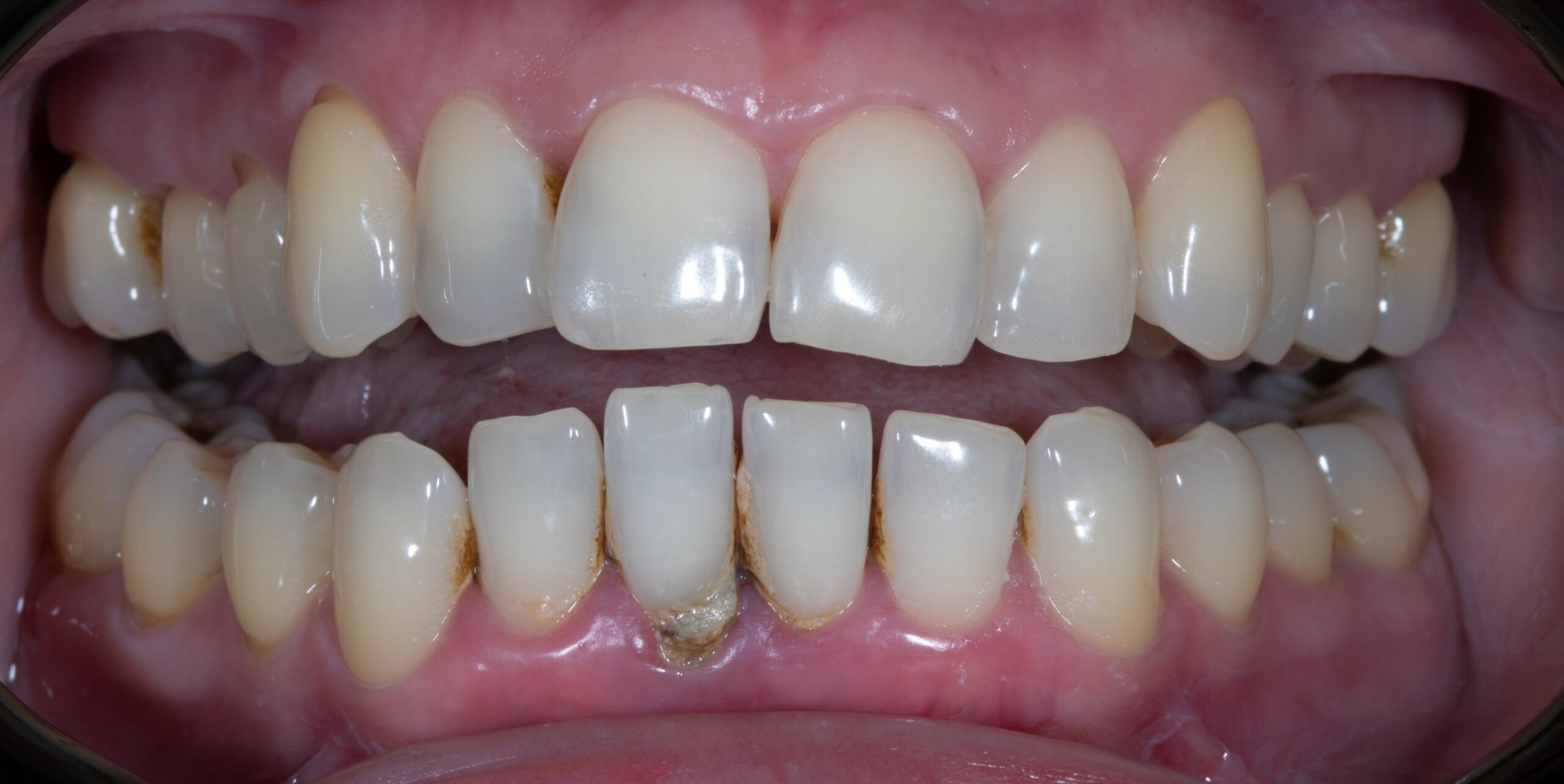
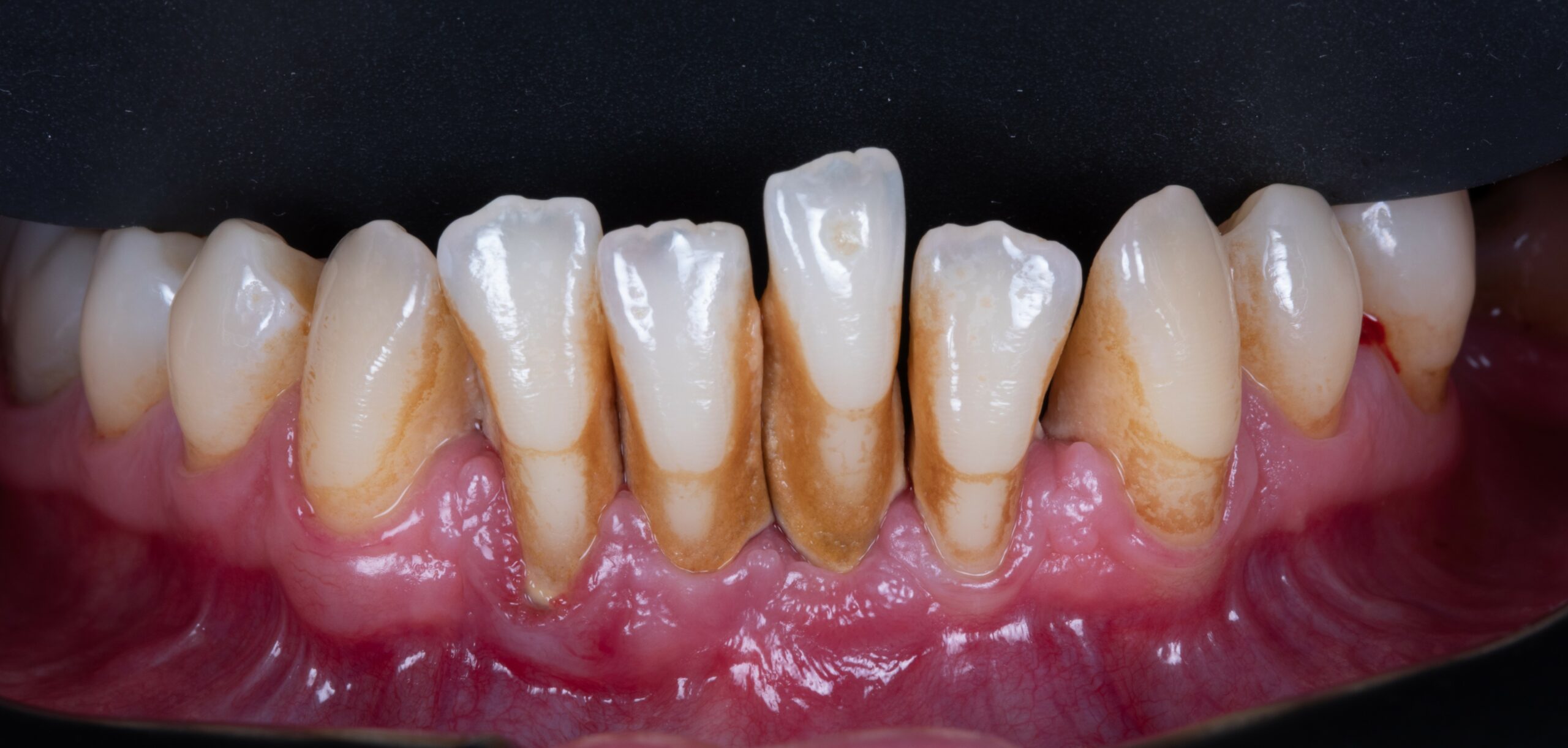
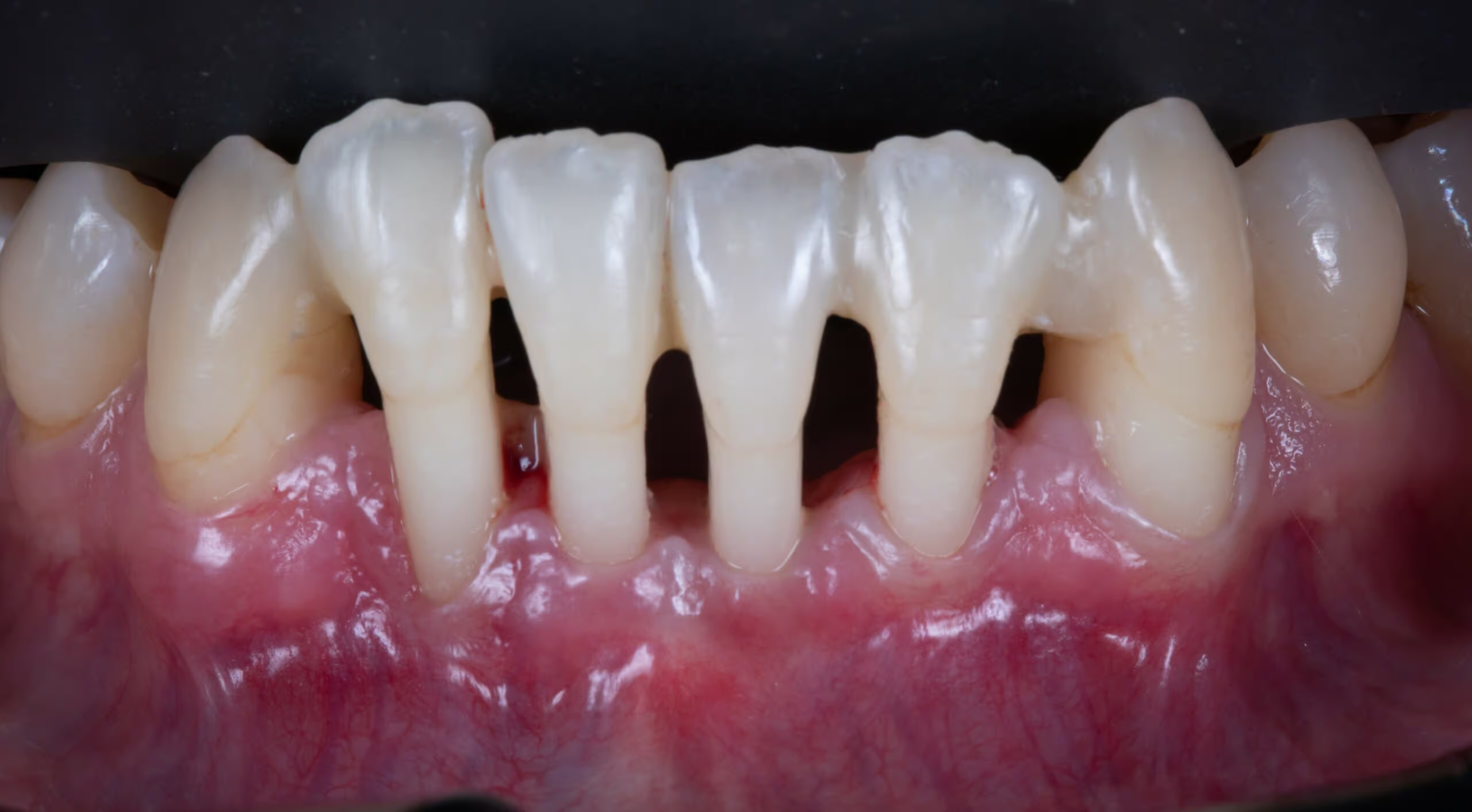
If you have suffered from gum disease, regular cleanings with an oral hygienist are necessary to maintain your health. This will prevent plaque and tartar from forming and ensure healthy gums in years to come!